There is a lot to consider during pregnancy, including testing for genetic conditions. This can often be an anxious experience for expecting parents, however prenatal testing and screening are incredibly important as they provide valuable information about your baby’s health.
Below are some common questions I receive from patients about tests like these, along with answers that will help prepare you for your first test or antenatal appointment with your obstetrician.
What is prenatal screening and testing? How is it different to diagnostic tests?
Prenatal screening is a broad term that refers to tests that are often recommended during pregnancy. This type of testing is non-invasive and reveals the risk of your baby having a particular genetic condition. Results are not definitive but can provide health professionals with guidance on whether further diagnostic tests are required.
Diagnostic tests may be more invasive and some may carry a risk of complications; they do however provide more accurate results and are recommended for mature mothers and those who have a family history of a genetic condition.
What are the main tests and when are they done?
First trimester
Prenatal testing can begin as early as 10 weeks and include the following:
- Non-invasive Prenatal Test (NIPT): a sample of blood is drawn from the mother and analysed to determine the risk of your baby having a chromosomal or genetic disorder.
- Ultrasound: shows the development of your baby. A dating scan shows how many weeks along you are. The nuchal translucency scan, undertaken at the 12-week mark, measures the amount of fluid accumulated at the back of your baby’s neck and can be used to calculate if your baby is at risk of chromosomal abnormalities.
- Blood tests: are done to check your health. They include checking your immunity to infective conditions like rubella, chickenpox and hepatitis. They also include testing for anaemia and identifying your blood group.
- Chorionic villus sampling (CVS): is a diagnostic test which can be carried out from 11 weeks. A CVS allows the doctor to collect a sample of cells from the mother’s placenta to analyse for genetic defects. It is usually only carried out in a pregnancy which has been identified as high risk for a genetic disorder.
Second trimester
Available tests include:
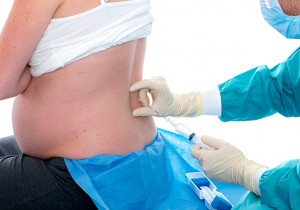
- Amniocentesis: may be recommended after a screening test has shown whether your baby has a high risk of a genetic abnormality. This involves collecting a small sample of fluid from the amniotic sac using a needle and is done under ultrasound guidance. Like CVS, this sample can then be used to determine the genetic makeup of your child.
- Morphology or anomaly ultrasound scan: is the most detailed scan of your baby that you and your obstetrician will receive. During this scan, we can visualise the fetal shape of your baby including the position of the placenta and the baby’s organs, to check that everything is growing correctly. The scan usually takes place around the 18-20-week mark and is often memorable as you may see the baby’s heart beating or the baby moving.
- Further blood testing: including checking for gestational diabetes which is done at the 24-28-week mark.
Third trimester
The most important care required during the third trimester is your regular antenatal appointments. Your obstetrician or midwife will check the baby is growing as expected and look for signs you are not developing complications such as preeclampsia. Should there be any concern, your obstetrician will arrange further blood or ultrasound scan tests.
At around 36 weeks, you may be offered a vaginal swab looking for Group B Strep, a bacteria that is found in one-third of all women. If identified, your obstetrician will give you antibiotics in labour to reduce the chance of your baby having a serious infection after birth.
Where do you take these tests?
The NIPT and early blood tests are available at most GPs. Though, after the 10-week mark, it is recommended to organise prenatal testing with your obstetrician who is trained to understand the results of the tests and can best inform you how they affect the ongoing pregnancy care.
How much do the tests cost?
Depending on your healthcare provider, out-of-pocket expenses for the first trimester can range from $450 to $500 and out-of-pocket expenses for the second trimester can range from $300-$400.
What happens if test results are positive for a genetic condition?
Learning that your unborn baby is at risk of having a genetic condition or birth abnormality and planning ahead for their future can lead to complex emotions including shock, grief and guilt.
In this situation, you and your partner should:
- Consult your obstetrician. As experts in this field, they can answer your questions or direct you to relevant resources, like a maternity support group.
- Consider genetic counselling, which provides further information to individuals and families about genetic conditions. They offer emotional and practical support on how to help people diagnosed with or at risk of a condition.
- Seek support from organisations like Perinatal Anxiety and Depression Australia (PANDA) that are trained in guiding expecting and new parents throughout pregnancy.
To give yourself the best care during this busy and emotional time, my advice is do not postpone or cancel your tests.
Dr Andrew Pickering is an obstetrician and gynaecologist with more than 20 years’ experience in high- and low-risk pregnancies, ensuring women and their families get the best, evidence-based obstetric and gynaecological care. He delivers babies at the Mater Hospital, North Sydney – one of Sydney’s leading maternity hospitals.