It can be scary to think about needing or wanting an epidural and what it will mean for you and your baby. Once you’re in labour, there’s no time for questions and research, but this article could help you to get the information you need to decide what’s right for your circumstances.
Epidurals provide unparalleled relief from the pain of labour and delivery. In what can be a long and drawn-out process, epidurals can be an absolute sanctuary from what can be an incomparable storm of pain.
What is an Epidural?
An epidural is a type of ‘regional anaesthesis’ – that means an anaesthetic that only works in a limited area. In an epidural, you will have an injection into the space that holds the nerves that connect to your belly, your pelvis and your legs. An epidural will numb those nerves and take the pain away when you’re in labour.
Taking the position
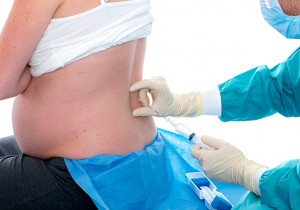
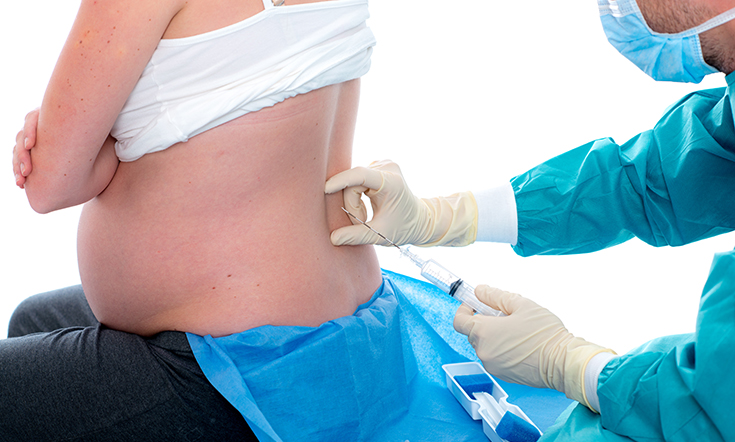
In order to reach the right nerves, your anaesthetist will need you to take up a particular position. You would need to curl over the side of the bed with your head tucked in, and your lower back pushed out. Don’t worry about remembering that though, the anaesthetist and nurses will help you.
Once you’re in the right position, the anaesthetist will give you local anaesthetic (which will stop you feeling the later injection) and then the epidural needle and the epidural catheter. After that’s all done, you will have a tube in your back so that you can get further doses of anaesthetic and pain-killing medications to make sure that the pain stays blocked.
Usually, the painkillers will be opioid-based medications such as morphine or fentanyl.
When is the right time?
It’s common to ask whether there’s a ‘right time’ to ask for your epidural. But, like everything in your pregnancy and labour, the answer is specific to you and your situation. The timing needs to be your informed choice, which is what makes early research important.
You might choose to have your epidural right at the start. You can have one as soon as you’re officially in labour (the doctor decides when that is). Or you can choose to have your epidural later in your labour if you feel you need it.
Some mums worry that they will ‘miss out’ on having an epidural if they ask too late. This does happen, but not often, especially for a mum having her first baby. However, if you’re having a fast labour it is possible to very quickly get to a point where your labour is just too advanced for the anaesthetist to safely give you an epidural.
If you are planning to have an epidural, make sure that you’ve discussed it with your birth partner and the medical team that will be in the room with you. You’re going to be very busy and distracted, which makes it important that everyone knows your wishes in advance.
Complications
It’s important to stress that epidurals have a very low risk of complications. They are extremely safe, practical, and effective medical interventions.
But, things can sometimes go wrong. The less serious complications include:
- a skin infection, bruising and irritation at the point where the needle goes in.
- low blood pressure (which happens to around one in 10 mums)
- dural puncture headaches, which happen to about one in every 150 mums. These happen when some spinal fluid leaks out when the needle goes in and you end up with severe and long lasting headaches.
The more serious and very rare complications include:
- nerve damage, which happens to around one in every 50,000 mums
- paraplegia, which happens to fewer than one in every 250,000 mums.
Disadvantages
There can be disadvantages to epidurals that you need to be aware of.
An inadequate or failed block:
- This can mean a less-than-perfect block where you can still feel some pain or discomfort in part of your body (around one in 10 mums experience this), or a total failure of the block (very rare, less than one per cent of all epidurals).
Nausea and vomiting:
- Some nausea is common during labour because of the pain, but epidurals also decrease your blood pressure, which can contribute to nausea and vomiting.
Maternal fever:
- It’s common for mums who have epidurals to also have fever during labour., but it doesn’t commonly lead to negative consequences.
Others:
- You might feel itchy at the injection site, but this is very rare.
What will an Epidural do to my Labour?
You hear a lot of stories from people who think epidurals are a bad idea, but an epidural’s biggest effect on your labour is to take away the pain.
This is what will happen;
- Epidurals either partially or completely impair your ability to move and use your legs, which means you will be bed-bound and unable to make big changes to your position for delivery.
- On average, there is a small increase in the likelihood of your needing either vacuum or forceps.
- Epidurals increase the chance that your baby won’t rotate into the perfect face-down position for labour. This can make vaginal delivery a bit more difficult.
- The second stage (the pushing stage) might be slightly longer with an epidural, less than 15 minutes is the average.
However, epidurals do NOT lengthen the time it takes for you to become fully dilated and do NOT significantly increase the risk of cesarean delivery.
What about my baby?
Epidurals are very safe for mum and for baby.
There is a tiny chance that there will be a transfer of the painkiller from you to your baby. Any transfer will be minimal and the risk of complications from this is very low.
Fewer than one in every 10 mums who have an epidural will experience an abnormally low foetal heart rate. If this happens, you will need to have intravenous fluids and change your position, but it passes, and doesn’t increase the risk of caesarean section.
Decide if an Epidural is right for you Before the Delivery Room
Getting through labour without pain relief is not a competition and there are no prizes. You do not have to be a martyr to be a mum. Make the decision that is right for you about whether or not to have an epidural – not the one that’s right for your mum, or your sister, or your best friend.
Make sure you have the information you need, and you’ve asked all the questions you need to before you go in to labour. What’s best for you is best for your baby.